Age Related Macular Degeneration
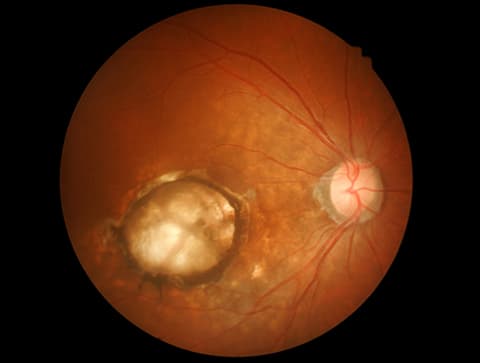 The macula accounts for a patient’s “central vision.” Age related macular degeneration is characterized by drusen (deposits under the retina), pigmentary changes, loss of retinal tissue, and hemorrhage on exam.
The macula accounts for a patient’s “central vision.” Age related macular degeneration is characterized by drusen (deposits under the retina), pigmentary changes, loss of retinal tissue, and hemorrhage on exam.
Symptoms of macular degeneration can include vision loss, metamorphopsia (distortion), micropsia (image size differences), and scotoma (blind spot).
Age related macular degeneration can be subdivided into dry macular degeneration and wet macular degeneration.
Dry macular degeneration is more common and usually occurs first. Specific exam findings for this condition include drusen, pigmentary changes, and retinal pigment epithelium atrophy (retinal tissue). This condition may be slowly progressive and vision loss primarily arises from loss of retinal tissue and photoreceptors (light sensing cells).
Therapy varies based on patient condition but include AREDS2 vitamins, self-monitoring with Amsler grid, and smoking cessation.
Wet macular degeneration occurs due to the growth of abnormal blood vessels called choroidal neovascularization. These vessels may leak fluid or cause hemorrhage (bleeding) under the neurosensory retina. When bleeding occurs this may lead to the formation of subretinal fibrosis (scar tissue). Prompt intervention in wet macular degeneration is essential in reducing the risk of permanent irreversible vision loss.
Treatments exist for wet macular degeneration. Most commonly this may be treated with an injection of medication into the eye. Medications include aflibercept (Eylea), bevacizumab (Avastin), and ranibizumab (Lucentis). Less commonly employed treatments include photodynamic therapy (PDT) and thermal laser.
Advanced retinal imaging including retinal angiography and optical coherence tomography are critical tools in diagnosing macular degeneration and following response to treatment.
The surgeons at Central Florida Retina are fellowship trained retina specialists practicing the latest treatments for macular degeneration. Should you be experiencing any of these symptoms or would like to request a consultation, please contact (800) 255-7188.



