Epiretinal Membrane
The retina is a light-sensitive tissue that lines the inside of the back of the eye. Your central vision is a small portion of the retina called the macula. When a small piece of scar tissue forms on the surface of the inner portion of the retina it is known as an epiretinal membrane (ERM). These can also be referred to as macular pucker or cellophane maculopathy. These membranes can put traction on the macula and may lead to pseudo holes or lamellar (layered) holes in the retinal tissue. These “holes” are not full thickness defects in the retinal tissue but still may affect your vision. Epiretinal membranes (ERM) are most common in patients greater than 50 years of age and affect men and women equally. The condition can affect both eyes in up to 25% of cases.
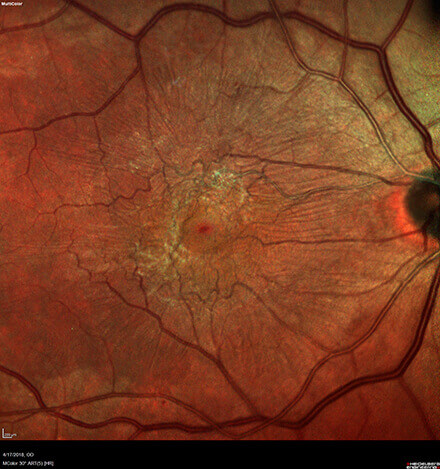
Causes:
The cause of ERMs is due to cellular changes (liberation of retinal cells on the surface of the retina) which can lead to the growth of a sheet of fibrous tissue on the retinal surface. This membrane may contract and cause traction (or pulling) and puckering of the retina, leading to decreased and wavy vision.
- Posterior Vitreous Detachment (most common association)
- As we age our vitreous gel shrinks inward and can put traction onto the retina in the macula which in some patients may lead to scar tissue formation.
- Diabetes
- Uveitis (inflammation in the eye)
- Retinal tears/detachments
- Retinal vein occlusions
- Trauma
Symptoms:
There is no way to predict who will develop an epiretinal membrane or when it will occur. Most patients who have epiretinal membranes are found incidentally and patients usually have no symptoms. There are no environmental or genetic links known to increase the risk of forming an ERM. Patients should look out for the following signs and symptoms.
- Blurred central vision
- Metamorphopsia (wavy or distorted vision)
- Double vision
- Image size discrepancies (smaller or larger)
The degree to which these symptoms will affect your vision will depend on the size and location of the membrane. If you notice any of these symptoms you should contact us immediately, at (800) 255-7188.
Diagnosis and Treatment:
A thorough dilated eye exam will be performed by your surgeon to help with the diagnosis and treatment of epiretinal membranes. An imaging test called optical coherence tomography (OCT) will be performed to get a detailed look at the macula looking for swelling, traction and other abnormalities in the macula. Some additional testing such as fluorescein angiography (FA) may be used to diagnose the underlying condition which caused the epiretinal membrane if deemed not from the vitreous gel separation.
Observation
If the ERM is very small or in early stages your surgeon will likely advise observation to see how the membrane progresses over time.
Pars Plana Vitrectomy
A microsurgical procedure used to remove the vitreous gel (floaters) with three small incisions in the white part of the eye (sclera). This is done in an operating room under a microscope which is used to help remove the scar tissue with very small instruments. Recovery time is generally 1-2 weeks.
In general, most epiretinal membranes can be followed over time without treatment as most lead to small or no changes in vision. If the membrane progresses, surgical intervention with vitrectomy will likely be necessary as there are no drops, nutritional substances or medications that will help to remove the membrane. The amount of vision restored after vitrectomy generally depends on the underlying cause of the membrane, the amount of traction of the membrane on the retina and how long it was present prior to surgery. Continued follow up with your surgeon is recommended to follow the improvements in retinal thickening and contour. At Central Florida Retina our physicians have been diagnosing and treating epiretinal membranes for over 40 years. For further information or to book an appointment call 800-255-7188.



