Diabetic Retinopathy
What is Diabetic Retinopathy?
Diabetic Retinopathy is one of the leading causes of vision loss in Americans. This is particularly true in the Southeastern United States, and especially in the metro Orlando area.
Diabetic retinopathy is the manifestation of Diabetes Mellitus in the retina, the light-sensing layer that lines the inside of the eye. As with the rest of the body, Diabetes, especially if not under great control, causes ongoing damage to the blood vessels that supply oxygen and nutrients to the retina, in the back of the eye.
The retinopathy from Diabetes can affect the eye in multiple ways. Often, the changes can develop and progress to an advanced state before causing noticeable symptoms in the vision. Thus, all patients with Type 1 or Type 2 Diabetes should get a dilated eye exam with an experienced primary eyecare provider EVERY YEAR.
Diabetic Retinopathy is described as Non-Proliferate or Proliferative. Both forms of Diabetic Retinopathy can result in vision changes.
Non-Proliferative Diabetic Retinopathy
This is the earlier stage of diabetic retinopathy. Vision-threatening changes in this state can arise from leaking blood vessels, which cause swelling of the retina (called diabetic macular edema), or from direct loss of blood flow to the retina. Many of these changes can be successfully treated by our specialist physicians with lasers or injections into the eye.
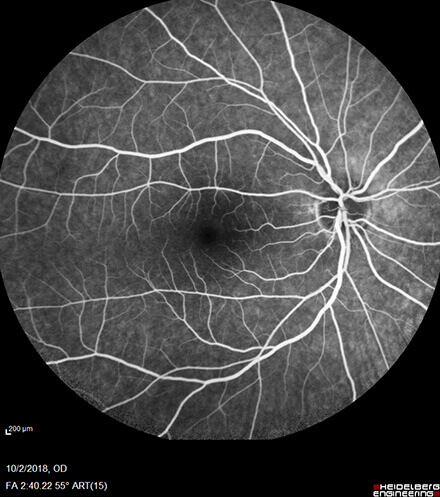
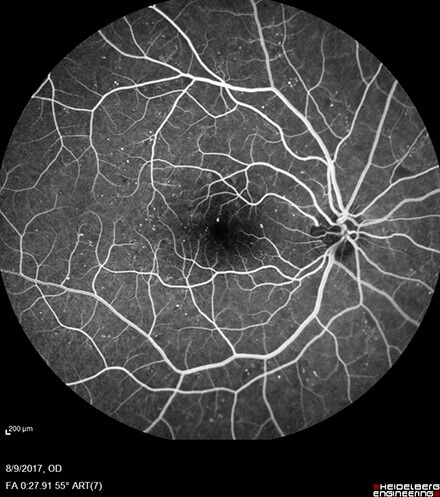
Proliferative Diabetic Retinopathy
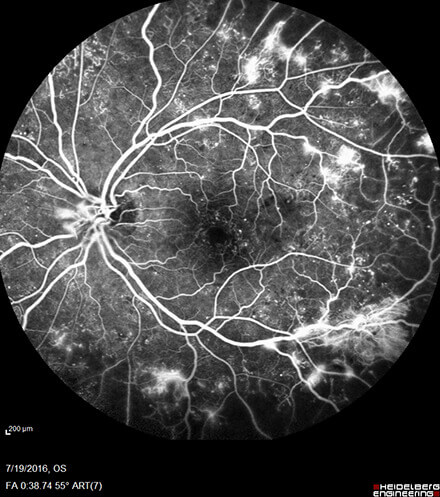
This is the more advanced stage of diabetic retinopathy, and once an eye reaches this stage, follow-up and treatments are very important. Some of the changes of this stage can include bleeding into the eye (vitreous hemorrhage) and the development of retinal detachments. Changes from proliferative diabetic retinopathy can cause significant vision loss. Lasers, injections, or surgery may be needed at this stage.
Unrecognized or untreated, diabetic retinopathy can be a blinding condition. Central Florida Retina physicians are some of the most experienced specialists in diagnosing and treating this condition. Please contact us if you have been told that you have diabetic retinopathy or if you feel you may need attention for this disorder.



